Curious about skin lesions? Explore DIY removal methods, natural remedies, and tips to achieve clearer skin and a better balance in your life.
Thank you for reading this post, don't forget to subscribe!Our skin is the largest organ of the body and a window into our health. One of the most common problems people face is the appearance of skin lesions.
Although many types of skin lesions are harmless, some can affect self-confidence or cause discomfort.
What Are Skin Lesions: How to Remove Skin Lesions Yourself
In the journey toward life balance, caring for your skin is more than just a beauty routine—it’s a form of self-respect and mindful living.
When your skin feels uncomfortable or looks unhealthy, it can impact your emotional equilibrium and how you move through the world.
By learning safe and natural ways to care for or remove certain skin lesions at home, you’re not only nurturing your outer appearance but also supporting your overall well-being and confidence.
This guide will help you understand what skin lesions are, which ones you can remove yourself, and how to do it naturally and safely—so you can feel more balanced and at ease in your own skin.
What Are Skin Lesions?

A skin lesion is a general term used to describe any abnormal growth or change in skin appearance.
These may appear as bumps, growths, spots, discoloration, or patches. Some skin lesions are present from birth, while others appear later due to a variety of reasons, such as:
- Skin infection
- Excessive sun exposure
- Hormonal imbalance
- Genetics
- Allergies
- Autoimmune conditions
- Natural aging
Skin lesions can be either primary (present on previously healthy skin) or secondary (evolving from an existing lesion).
Common Types of Skin Lesions:
- Warts
- Skin tags
- Moles (small benign ones)
- Milia (tiny white bumps)
- Seborrheic keratosis
- Keratosis pilaris
Some lesions pose cosmetic concerns, while others can be a sign of underlying health issues—such as skin cancer. That’s why it’s critical to understand what type you’re dealing with before trying to remove it.
Types of Skin Lesions You Can Remove at Home
Not all skin lesions are safe to remove yourself. However, some common, benign, and superficial types can be addressed with home remedies and over-the-counter solutions.
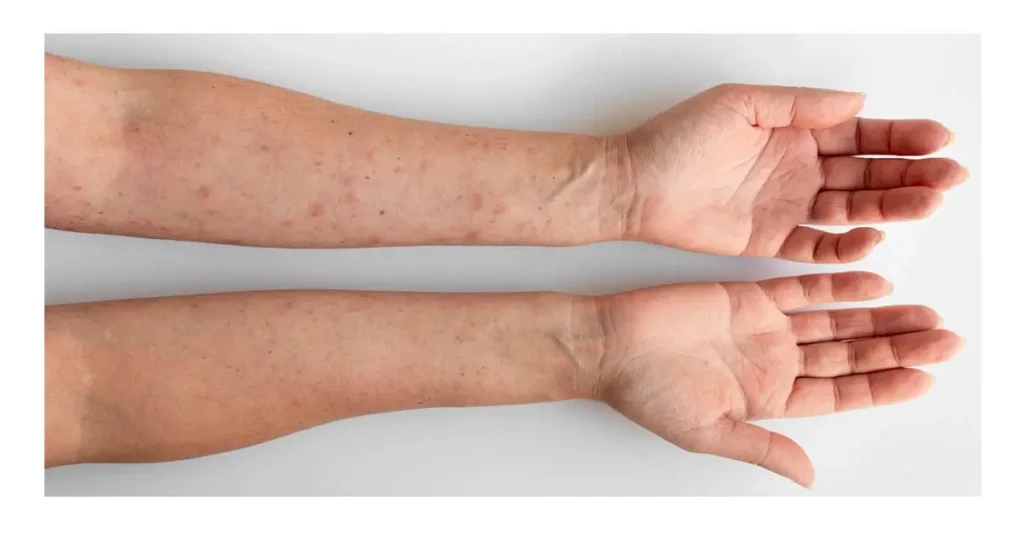
1. Skin Tags
Small, soft, painless tags of skin that often appear on the neck, armpits, eyelids, or under the breasts.
2. Warts
Caused by the human papillomavirus (HPV), these rough, raised bumps can occur anywhere on the body, especially hands, feet, and face.
3. Benign Moles
Small, flat or raised moles that remain uniform in shape, size, and color may be removed naturally—but only after ruling out malignancy.
4. Milia
Tiny, hard white bumps (cysts) occur mostly around the eyes, cheeks, and forehead.
5. Seborrheic Keratosis
Non-cancerous, waxy, wart-like growths that may occur with age.
Important Note: Always have suspicious or new skin lesions checked by a dermatologist. Never attempt to remove lesions that are bleeding, growing rapidly, irregular in shape, painful, or changing in color.
When NOT to Remove Skin Lesions Yourself
Safety should always come first. DIY removal is not recommended for all types of lesions. Avoid self-removal in the following cases:
- Lesions with irregular borders, color changes, or asymmetry
- Lesions that bleed or ooze
- Quickly growing or changing moles.
- Lesions located in sensitive areas such as the eyelids, lips, or genitals
- If you have a history of keloids or scarring
If you see any of the above warning signs, consult a dermatologist for a proper diagnosis and treatment plan.
Safe and Natural DIY Methods to Remove Skin Lesions
Once you’ve identified that your skin lesion is safe to remove at home, you can explore natural remedies. These solutions are especially popular for removing skin tags, warts, and some moles.
Here are the most effective home-based methods:
1. Apple Cider Vinegar
A powerful antimicrobial agent, apple cider vinegar is one of the most popular choices for removing skin lesions.
How to Use:
- Soak a cotton ball in unfiltered, raw apple cider vinegar.
- Apply it directly to the lesion.
- Secure with a bandage and leave overnight.
- Repeat daily for 1–2 weeks.
The lesion darkens and falls off as the tissue is broken down by apple cider vinegar.
Note: If your skin is sensitive, do a patch test first to prevent irritation.
2. Tea Tree Oil
Tea tree oil is effective for warts and skin tags due to its antiviral and antifungal properties.
How to Use:
- Use one teaspoon of a carrier oil (such as coconut or olive oil) to dilute two drops of tea tree oil.
- Apply gently to the lesion with a cotton swab.
- Repeat 2–3 times daily until the lesion shrinks and falls off.
Tea tree oil is safe and soothing, but avoid getting it near your eyes or mouth.
3. Banana Peel
Banana peels are often used as a folk remedy for wart removal due to their potassium and enzyme content.
How to Use:
- Apply the inside of a fresh banana peel to the wart.
- Tape a small piece of peel over the lesion and leave it overnight.
- Repeat for 1–2 weeks.
The enzymes and moisture help soften and dissolve the lesion over time.
4. Iodine Solution
Iodine is highly effective in drying out skin tags when applied externally.
How to Use:
- Clean the area with soap and water.
- Apply liquid iodine directly to the tag with a cotton swab.
- Cover with a bandage.
- Repeat twice daily until it falls off.
Caution: Avoid using iodine if you have thyroid issues or iodine sensitivity.
5. Castor Oil and Baking Soda Paste
Baking soda and castor oil, a natural remedy, combine to create a potent paste that can remove minor wounds.
How to Use:
- To make a paste, combine baking soda and castor oil in a 1:1 ratio.
- Apply the paste to the lesion.
- Cover with a bandage and leave overnight.
- Repeat daily for 1–2 weeks.
This method is gentle and works especially well for benign moles and skin tags.
Over-the-Counter Treatments
In addition to natural methods, several over-the-counter (OTC) treatments can help safely remove warts and skin tags.
Cryotherapy Kits
These freezing kits use liquid nitrogen or similar compounds to freeze off warts or tags. They’re easy to use at home and deliver fast results.
Salicylic Acid Solutions
Commonly sold as gels, patches, or liquids, salicylic acid helps peel away layers of warts over time.
Tip: Follow instructions carefully and protect surrounding skin when using OTC acids.
Aftercare Tips
Once you’ve removed a skin lesion, proper aftercare is essential to prevent infection and scarring.
- Keep the area clean and dry.
- Use a healing ointment, such as aloe vera or an antibiotic cream.
- Avoid sun exposure (use sunscreen)
- Avoid picking or scratching the treated area.
- Monitor for signs of infection, such as redness, swelling, or pus.
Potential Risks and Side Effects
While home treatments can be effective, they’re not risk-free. Be aware of the potential side effects:
- Infection if tools or products aren’t used properly
- Scarring, especially from aggressive removal methods
- Pain or irritation
- Incomplete removal (lesion may regrow)
Always start with gentler remedies and watch for signs of adverse reactions.
Why Skin Health Matters for Life Balance
Your skin is more than just a physical barrier—it’s a reflection of your inner health and emotional well-being.
When you’re bothered by skin lesions or discomfort, it can affect your confidence, self-image, and even your daily interactions.
Taking control of your skin health through safe, natural methods not only supports your physical wellness but also brings peace of mind.
By choosing gentle, intentional care for your skin, you are practicing self-respect and creating a more grounded, balanced version of yourself—inside and out.
When to Consult a Dermatologist
Not all lesions can or should be managed at home. Reach out to a skincare professional if:
- The lesion appears suspicious or is rapidly changing.
- You’re unsure of its type.
- Home remedies haven’t worked.
- The lesion is large, deep, or causing discomfort.
Dermatologists offer advanced treatments like laser therapy, electrosurgery, and surgical excision for safe, permanent removal.
FAQs
Q. How to remove skin lesions yourself?
You can remove certain types of skin lesions yourself, such as skin tags, warts, and some small benign moles.
Popular natural therapies include castor oil combined with baking soda, apple cider vinegar, and tea tree oil.
Over-the-counter treatments like cryotherapy kits and salicylic acid are also effective.
However, always be sure to identify the type of lesion before attempting removal. Avoid home removal if the lesion is irregular, painful, or rapidly changing in size or color. When in doubt, consult a dermatologist for a professional opinion.
Q. How to clear up skin lesions?
Clearing skin lesions depends on their type and cause. Mild lesions like acne, milia, or keratosis pilaris can be treated with exfoliation, gentle cleansers, moisturizers, or topical creams containing ingredients like salicylic acid or retinoids.
For infectious lesions like warts, natural remedies or OTC wart removers may work. Avoid picking or scratching the affected area, and keep it clean.
For long-lasting or spreading lesions, a medical consultation is recommended to rule out infections or underlying skin conditions.
Q. How to get rid of skin lesions naturally?
Apple cider vinegar, tea tree oil, or iodine solution applied directly to the lesion are examples of natural remedies for skin lesions.
These work by drying out or breaking down the tissue. Banana peels, aloe vera gel, and turmeric paste are traditional remedies known to soothe and heal certain lesions.
Most natural treatments require consistent daily application for a few weeks. Always perform a patch test to assess sensitivity and consult a professional before trying any remedy on growths with irregular shapes or colors.
Q. Can skin lesions go away on their own?
Some skin lesions, such as mild rashes, small warts, or insect bites, may resolve on their own as the skin heals. However, others, like skin tags, moles, or seborrheic keratosis, usually persist unless removed.
Certain lesions caused by viral infections may take weeks or months to resolve. It’s important to monitor any lesion for changes and avoid assuming it will disappear without cause. If you notice growth, pain, itching, or bleeding, seek medical advice.
Q. Can you remove a lesion?
Yes, many lesions can be removed, especially if they are benign. Dermatologists offer various professional treatments, such as cryotherapy, laser removal, or minor surgery, for safe, scar-free results.
At home, you can remove small growths such as warts or skin tags using natural remedies or OTC products. Proper identification of the lesion is critical before removal, as some can be dangerous if self-treated.
Always consult a doctor if you’re unsure or if the lesion appears suspicious.
Q. How to get 100% clear skin?
Achieving 100% clear skin involves a combination of consistent skincare, healthy habits, and lifestyle changes. Start with a gentle routine that includes cleansing, exfoliating, and moisturizing.
Choose products with ingredients such as niacinamide, salicylic acid, or vitamin C to target specific issues.
Eat a nutrient-rich diet, stay hydrated, and reduce stress for healthier skin from the inside out. Avoid touching your face and use sunscreen daily.
For persistent issues or scarring, seek professional guidance from a dermatologist.
Conclusion
Skin lesions are common and, in many cases, harmless. Thanks to nature and modern medicine, you can safely remove certain types of lesions at home—like warts, skin tags, and benign moles.
Taking the time to care for your skin is an act of self-care that aligns with balanced living.
When you address even small concerns, such as skin lesions, you’re not just attending to your physical body but also supporting your mental clarity, confidence, and peace of mind.
It’s a gentle reminder that living in balance means honoring your body from the outside in.
Get more LIFE BALANCE TIPS.
You might like to read:

